Old Vaccine Brings India New Hope in Fight Against Leprosy

India’s decision to conduct new trials on the world’s first leprosy vaccine is eliciting hope it will help eliminate the dreaded disease from the country.
Following a declaration by the World Health Organization (WHO), India has been officially counted as a leprosy-free country since 2005, meaning less than one person in 10,000 people is afflicted with disease. Many experts, however, say the true rate of infection is much higher, accounting for more than 60 percent of the world’s new cases.
Indian authorities recently announced they would soon roll out an advanced field implementation trial of the vaccine Mycobacterium Indicus Pranii, or MIP.
“In the early field trials of the MIP, the vaccine’s protective efficacy was found to be quite encouraging, with 68.6 percent of people being protected for four years and 59 percent being protected for eight years.
This vaccine also expedites cure rates to people already infected with the disease,” said Dr. Utpal Sengupta, a leading New Delhi-based leprosy researcher, who has worked in the field for more than four decades. “It has the ability to bolster India’s new campaign, which aims to eliminate leprosy as a public health problem by 2020.”

Leprosy patient Gopal Bag, 62, sits with his amputated right leg at the Leprosy Mission Trust India hospital, Kolkata, Sept. 20 2016. Bag now has claw hands and toes as a result of the infection having gone untreated for years. (M. Hussain/VOA)
Field trial to start soon
The soon-to-be-launched field trial in five high-endemic districts of Bihar and Gujarat will be administered to people with leprosy and those in close physical contact to them, in combination with the common anti-leprosy drug Rifampicin.
In a statement, Dr. Soumya Swaminathan, the director-general of the Indian Council of Medical Research, which is working with the government on the rollout of the MIP trial, said the government has embarked on a “multi-pronged attack” on leprosy.
He added the campaign will increase “active case detection,” saying it could be the key to eliminating the disease, “hopefully in the next five to 10 years.”
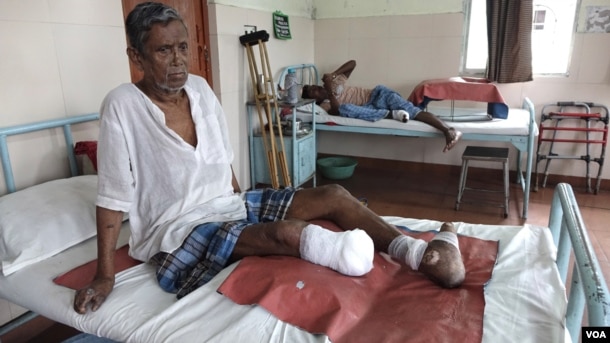
«There was no awareness about the disease when I got the infection. Now I know, if I took the treatment early I would have not faced this amputation or any disfigurement,» Bag said. (M. Hussain/VOA)
India still hotbed
Modern medical advancements have largely diminished the impact of leprosy, mostly eliminating the disease globally but India still accounts for a majority of the world’s new cases.
Pointing to the last available data released in 2013, when India had more than 135,000 new cases, experts warn that new infections are rising.
In the 1980s, Indian researcher Gursaran Prasad Talwar developed the MIP vaccine at India’s National Institute of Immunology.
In 2005, the results of a field trial in northern India were found to be extremely promising, but with the WHO declaring India leprosy-free that year, the MIP soon went out of focus.
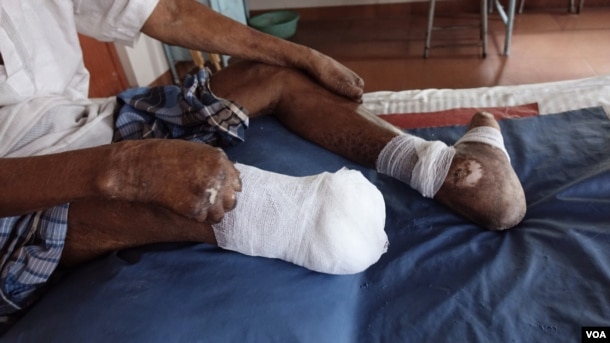
An amputated leg, claw toes and claw hands of leprosy patient Gopal Bag are seen at the Leprosy Mission Trust India hospital, Kolkata, Sept. 20 2016. (M. Hussain/VOA)
Infections rise after WHO declaration
Some believe the 2005 WHO declaration ended up triggering a rise in the number of new cases.
“Before India was declared leprosy-free, in the country there was a dedicated system to detect the leprosy cases and provide medical care to them. But, after 2005, when the leprosy treatment was integrated into the general health care services, the process of active case search was abandoned,” said Dr. Helen Roberts, superintendent of the Leprosy Mission Trust India Hospital.
“Since the designated system for leprosy virtually became dysfunctional after 2005, the cases of new infections in the country have gone up and cases remaining untreated for years, we have seen a rise in physical disabilities.”
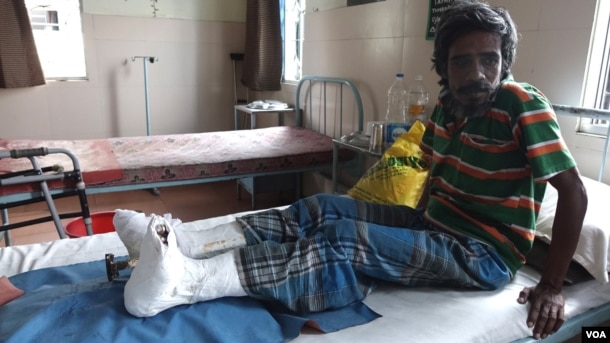
A leprosy patient, who has undergone corrective surgery of his claw toes, is recuperating at the Leprosy Mission Trust India hospital, Kolkata, Sept. 20 2016. (M. Hussain/VOA)
Need for awareness campaign
Dr. Jerry Joshua, a surgeon at the Leprosy Mission Trust India, said that a strong awareness campaign is needed to help detect the infections early and get them treated.
“Early detection actually hinges upon getting people to know what the disease is all about. It’s about spreading the knowledge about the disease and the knowledge that leprosy should be detected early. People should know what are the signs and symptoms of leprosy, what are dangerous symptoms and what are the disease’s early signs and symptoms,” Joshua told VOA.
Experts agree that many private doctors and clinics do not provide data on leprosy patients to the health authorities, so the true figure on infections does not show up in statistics.

A worker is designing special shoes for leprosy patients at the Leprosy Mission Trust India hospital, Kolkata, Sept. 20 2016. (M. Hussain/VOA)
Stigma suppressing real numbers
«Fearing stigma, which is attached to the disease, many leprosy patients maintain secrecy about their infection in India,» Subhash Chandra Ghosh, who runs a leprosy care NGO in a leprosy-endemic area of West Bengal’s West Midnapur district, told VOA.
«They avoid visiting government-run other special leprosy care hospitals where, they fear, the information of their infection would become public. They choose to go to private clinics and fall off the radar of the health authorities,» Ghosh said.
«The actual number of leprosy infections in India could be in fact three or four times higher than the figures provided by the authorities. Unless the government take some solid strategic steps to uncover this hidden leprosy population, fight to eliminate leprosy will be an uphill task.»
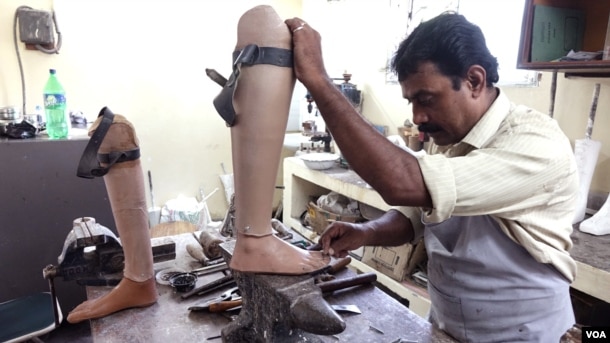
A worker is designing a prosthetic leg for a leprosy patient at the Leprosy Mission Trust India hospital, Kolkata, Sept. 20 2016. (M. Hussain/VOA)

